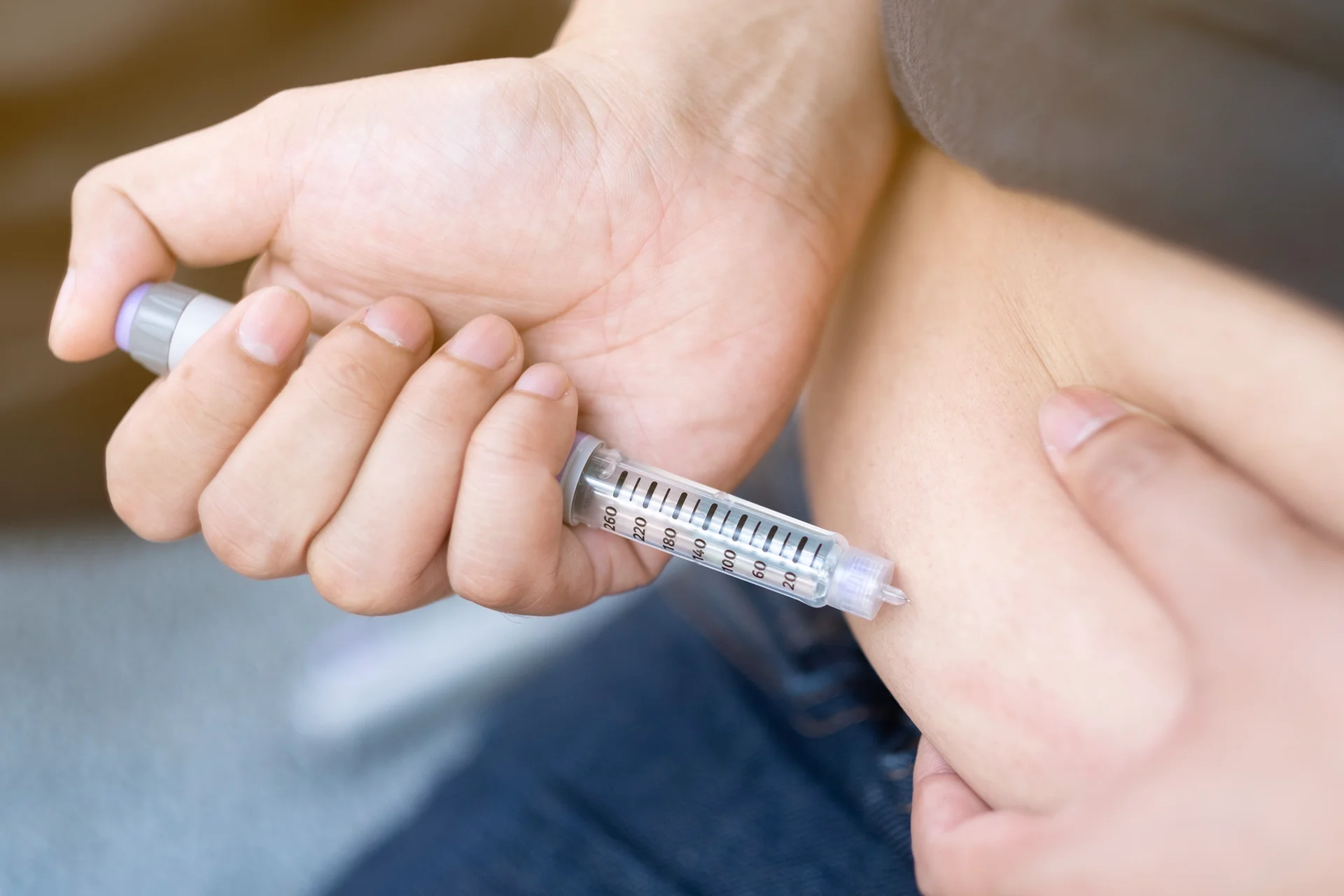
BCBS coverage for Ozempic for weight loss varies by policy and state. Confirm with your specific BCBS plan for eligibility and coverage details.
Ozempic, a medication primarily used to manage type 2 diabetes, has gained attention for its weight loss benefits. As a content writer focusing on practical and search-engine optimized information, it’s essential to understand that insurance coverage for medications can be complex and differs widely.
Blue Cross Blue Shield (BCBS), one of the largest health insurance networks, offers various plans that may cover Ozempic, but this depends on individual policy details and the intended use of the medication. Patients considering Ozempic for weight management should consult their healthcare providers and contact their BCBS representative to verify if their particular plan provides coverage for this medication. By navigating the nuances of health insurance, you can make informed decisions about your weight loss journey and potential medication use.
Bcbs And Medication Coverage Policy
Understanding your health plan’s medication coverage is key. Blue Cross Blue Shield (BCBS) offers various policies. These may include coverage for medications like Ozempic, often prescribed for weight loss. Let’s dive into how BCBS decides on covering specific drugs.
Criteria For Medication Approval
BCBS uses strict rules for medication approval. They check safety, effectiveness, and cost. Your doctor must prove the need for a particular medication. Prior authorization may be required. This means you need approval before BCBS covers the drug.
- Diagnosis confirmation
- Previous treatments tried
- Clinical guidelines met
- Potential side effects considered
The Role Of Formulary Lists
A formulary is a list of drugs a health plan covers. BCBS updates its formulary regularly. Drugs are grouped based on tier levels. Ozempic’s inclusion depends on its tier and your specific plan. Check the formulary list on BCBS’s website or contact them directly.
| Tier | Drug Type | Cost to You |
|---|---|---|
| 1 | Generic | Lowest |
| 2 | Preferred brand | Moderate |
| 3 | Non-preferred brand | Higher |
| 4 | Speciality drugs | Highest |
Review the list to see if Ozempic falls within your benefits. Always double-check with BCBS for the most accurate information.

Credit: www.singlecare.com
Ozempic: A Brief Introduction
The world of weight management and diabetes treatment has encountered a new ally – Ozempic. Known scientifically as semaglutide, Ozempic emerges as a promising solution for adults grappling with these health concerns.
Understanding Ozempic’s Usage
Ozempic serves multiple purposes, primarily focusing on improving blood sugar levels. People with type 2 diabetes often turn to this medication under medical advice. It mimics a hormone called GLP-1 to trigger insulin production. This process helps regulate blood sugar levels effectively. But there’s more to Ozempic than meets the eye.
Ozempic isn’t just for diabetes. Given its influence on bodily functions, its usage extends to weight management for certain patients. Doctors may prescribe it to control weight, but always within a larger treatment plan that includes diet and exercise.
Data On Ozempic And Weight Management
Clinical trials have shown promise in Ozempic’s role in weight loss. Here’s a snapshot of the findings:
| Study | Weight Loss Outcome |
|---|---|
| STEP 1 | Participants lost up to 14.9% body weight |
| STEP 2 | Up to 10% reduction noted in a year |
These figures indicate a significant impact when Ozempic forms part of a comprehensive health strategy. Reports suggest marked improvements in not only weight metrics but overall health markers among users.
Before considering Ozempic for weight loss, verifying insurance coverage is crucial. Does BCBS cover Ozempic for weight management? Coverage may vary based on individual health plans and medical necessity. Patients should check with their specific Blue Cross Blue Shield policy for details on Ozempic coverage.
Navigating Insurance For Weight Loss Treatments
Navigating insurance for weight loss treatments often feels like walking through a maze. With obesity rates rising, many seek medical aid to manage their weight. Insurance coverage varies, and understanding your policy is crucial. Specifically, does Blue Cross Blue Shield (BCBS) cover Ozempic for weight loss? Let’s unravel the complexities of insurance coverage for this treatment option.
Consideration Factors For Coverage
Finding out if BCBS provides coverage for Ozempic starts with dissecting your policy. Policies have unique terms, and certain conditions influence coverage eligibility. Important factors include medical necessity, your plan’s formulary, and prior authorizations.
Key consideration factors:- Prescribing doctor’s recommendation: Essential for proving medical necessity.
- Plan specifics: Coverage differs across plans.
- Formulary status: Check if Ozempic is on your plan’s drug list.
Contact your BCBS representative for personalized guidance. They can clarify coverage aspects and the process for submitting claims or prior authorization requests.
Weight Loss Treatments: Special Cases
Certain situations require a deeper dive when seeking insurance coverage for weight loss treatments like Ozempic. For instance, if obesity correlates with other health issues such as diabetes, coverage may differ. Understanding these nuances is key.
Special cases to consider:- Coexisting conditions: Coverage might extend if weight loss benefits another diagnosed condition.
- Variation across states: Insurance mandates can vary by state.
- Appeal processes: If initially denied, knowing how to appeal is important.
Document all interactions with your insurer and healthcare provider. This ensures you have a paper trail if you need to appeal a denial of coverage.
Examining Bcbs Stance On Ozempic
Many people ask if their health insurance covers weight loss treatments like Ozempic. The answer isn’t simple. It can depend on the insurance plan. One big name in health insurance is Blue Cross Blue Shield (BCBS). Let’s find out what BCBS has to say about Ozempic for weight loss.
Coverage Variances Across States
BCBS plans differ by state. This means that Ozempic coverage changes depending on where you live. Some states may cover it under certain conditions. Others might not cover it at all. We have to look at each state’s specific BCBS plan.
Important points to note:
- Check your state’s BCBS plan for details on Ozempic coverage.
- Look for specific conditions that might allow coverage for weight loss.
- Understand the requirements you must meet to get coverage.
Real Examples Of Coverage Decisions
Seeing real cases helps us understand Ozempic coverage better. Below is a table with examples:
| State | BCBS Plan | Ozempic Coverage for Weight Loss |
|---|---|---|
| Florida | Florida Blue | Yes, with prior authorization |
| Texas | BCBSTX | No, not covered for weight loss |
| California | Blue Shield of California | Limited, specific criteria apply |
Things to remember:
- Prior authorization might be needed for coverage.
- Each state has its own criteria for weight loss medication coverage.
- Doctor’s prescriptions might influence the decision.
Steps To Determine Your Coverage
Understanding insurance benefits can be tricky. For those considering Ozempic for weight loss, knowing if Blue Cross Blue Shield (BCBS) provides coverage is crucial. Follow the steps below to learn more about your specific plan benefits.
Contacting BCBS RepresentativesContacting Bcbs Representatives
Start by getting in touch with BCBS directly. Representatives are on standby to assist with coverage inquiries. Use the customer service number found on the back of your insurance card to reach out. Be ready with your plan details and membership ID. A representative will help verify if Ozempic is part of your prescription benefits.
Reading Your Policy’s Fine PrintReading Your Policy’s Fine Print
Every insurance policy has its own set of terms. Grab your policy booklet or log in to your online account. Look for sections on prescription coverage and exclusions. Search for ‘Ozempic’ or ‘weight loss medication’ to identify relevant clauses. Take notes on any copayments, deductibles, or limits that may apply. This exercise will help clarify the extent of your coverage.
Credit: www.singlecare.com
Prior Authorization And Ozempic
Navigating insurance coverage for medications can be complex. Especially with Ozempic, a prescription drug typically used for managing type 2 diabetes. But, did you know some people use Ozempic for weight loss? Whether Blue Cross Blue Shield (BCBS) covers Ozempic for weight loss depends on your policy. Prior authorization might be a crucial step.
The Process Explained
Prior authorization is insurance speak for getting a green light before starting a treatment. It means your insurer, like BCBS, needs to approve Ozempic before they agree to pay for it.
- Your doctor sends a request to BCBS.
- BCBS reviews the need for Ozempic.
- If approved, you get coverage following your plan details.
- Without approval, you may face higher out-of-pocket costs.
Tips For A Successful Prior Authorization Request
- Ensure your doctor fully understands your weight loss needs.
- Ask your doctor to provide your full medical history to BCBS.
- Check if BCBS needs more info about your weight loss journey.
- Follow up promptly with any requests from BCBS.
- Be aware of deadlines and respond to BCBS quickly.
Prior authorization can seem daunting, but with the right approach, you can streamline the process. Keep records of all communications and stay in touch with your doctor and BCBS.
Appealing A Coverage Denial
Appealing a coverage denial might feel overwhelming, but it’s a right every policyholder has. Suppose Blue Cross Blue Shield (BCBS) denies coverage for Ozempic as a weight loss treatment. Knowing the steps to challenge this decision can help secure the medication you need. Empower yourself by understanding your rights and how to navigate the appeal process effectively.
Understanding Your Rights
Understand insurance policies and your entitlements when a claim gets denied. Every insured individual holds the right to question and appeal decisions made by their insurance provider. This includes coverage for medications like Ozempic, which might be crucial for your health.
The Appeal Process: A Step-by-step Guide
- Review the Denial Letter: Start by thoroughly reading the denial letter from BCBS. Identify the reasons for Ozempic’s coverage denial.
- Gather Supporting Documents: Collect all relevant health records, a prescription from your doctor, and any literature supporting Ozempic for weight loss.
- Submit a Written Appeal: Craft a clear and concise appeal letter. Detail why Ozempic is necessary for your health alongside your supporting documents.
- Follow-Up Consistently: Keep track of your appeal’s status. Regular follow-ups can be essential to ensure a timely review.
- Understand the Timeline: Insurance providers, like BCBS, have specific time frames to respond to appeals. Note these timelines and be proactive throughout the process.
- Seek External Review: If your appeal is not successful, request an independent review by a third-party.

Credit: jetmedicaltourism.com
Alternatives If Bcbs Denies Coverage
Learning that BCBS does not cover Ozempic for weight loss can be disappointing. Yet, this isn’t the end of the road. Explore other options to support your weight loss journey. Below, find alternative medications and strategies to help you achieve your goals.
Other Medications For Weight Loss
If Ozempic is not an option, consider these medications:
- Phentermine: A short-term appetite suppressant.
- Orlistat: Reduces fat absorption from food.
- Naltrexone-Bupropion: A combo that controls cravings.
Each drug comes with its pros and cons. Speak with a healthcare provider to find the right choice for you.
Lifestyle Modifications And Support Systems
Make changes to your lifestyle for long-term benefits:
- Healthy Eating Habits: Embrace a balanced diet.
- Regular Physical Activity: Aim for at least 150 minutes a week.
- Sleep: Get 7-9 hours of quality sleep nightly.
Join support groups or seek a nutritionist for added guidance. Surround yourself with a positive network to stay motivated.
Future Of Obesity Treatment Coverage
The landscape of health insurance coverage for obesity treatments like Ozempic is ever-evolving. It is a critical focus for patients, healthcare providers, and insurers. As obesity rates climb, so does the demand for effective treatment options. Coverage for weight loss medications like Ozempic, often known for its diabetes treatment capabilities, is becoming a hot topic in the healthcare insurance industry.
Trends In Healthcare Insurance
Health insurance providers are recognizing obesity as a serious health condition. This condition leads to various comorbidities. Current trends suggest a shift in policy. Insurers are beginning to view weight loss treatments as a necessity rather than a luxury. Plans like Blue Cross Blue Shield (BCBS) scrutinize the effectiveness and cost of medications. Ozempic, specifically for weight loss, currently requires specific criteria for coverage.
- Expanding policy coverage for anti-obesity drugs
- Acknowledgment of weight loss treatment as preventive care
What Changes May Lie Ahead
In the near future, the paradigm of obesity treatment coverage might experience significant shifts. With drugs like Ozempic making headlines, here’s what could be in store:
- Wider acceptance of obesity as a treatable condition
- Insurers potentially reclassifying obesity treatments under essential benefits
- Lowered criteria thresholds for medication eligibility
BCBS may update their policies in response to healthcare trends and patient advocacy. It could lead to improved coverage of Ozempic for weight loss. Stay informed about your insurance plan. Speak to your healthcare provider about the best treatment for your situation.
Frequently Asked Questions
Will Insurance Cover Ozempic For Weight Loss?
Insurance coverage for Ozempic for weight loss can vary. Consult your provider to determine if your plan includes this medication for obesity treatment.
Are Any Weight Loss Drugs Covered By Insurance?
Some weight loss medications may be covered by insurance, depending on the provider and specific policy. It’s important to verify coverage with your insurance company.
Why Is Ozempic Denied By Insurance?
Ozempic may be denied by insurance due to lack of coverage for the medication, unmet pre-authorization requirements, or it not being on the insurer’s formulary. It could also be because cheaper alternatives are available. Always check your plan’s specifics for clarification.
Does Anthem Bcbs Cover Wegovy For Weight Loss?
Anthem BCBS may cover Wegovy for weight loss, but coverage varies based on individual plans and medical necessity. Always verify with your specific policy.
Conclusion
Navigating insurance coverage can be complex, especially for medications like Ozempic used off-label. BCBS may offer coverage depending on individual policy details and prescribing reasons. It’s essential to consult with your physician and insurance provider to understand your options. Being well-informed eases the journey towards effective weight loss management and optimal health.